Highs and Lows: The High
A Two Part Story
This job is full of highs and lows. Calls that go well, calls that don’t, people that live and people that die. This is a story about a day that I experienced both. This is a true story, told as best that I can recall it. At the time this story took place, I had been a Paramedic for about 4 months. I hope you enjoy it.
It’s a warm October day in rural Oklahoma, as summer has faded and the temperature drops slowly. It’s still warm enough to swim, so the area pools are still open in spite of the changing leaves. My guess is, that won’t last much longer, but let the kids have their fun. Leave it to the universe, however, to use this time to claim a last few victims…mine was one of them.
My partner, Tabitha, and I are on day two of a seventy-two hour shift and up to this point it’s been average, run of the mill stuff. General sickness, weakness, vomiting, and the occasional dialysis run. I’ve just gotten good and asleep for an afternoon nap when the pager beeps, rudely awakening me from my exhaustion induced slumber. The radio crackles, “Comms to 16, priority one. Rt 66 for palpitations, 26 year old female complains of chest pain. Time out, 1330 hours”.
Begrudgingly, I throw my uniform shirt on, stomp my feet into my boots, and head for truck. My partner is already in it, lights on, ready to go. I mumble some expletive under my breath, like usual on shifts like these, and away we go. On the way, we preplan: Monitor, 12 lead immediately, get her in the ambulance. Treat based on findings. ‘Probably bullshit. Usually is'.’, says my subconscious, but we’ll see.
We arrive on scene and the fire department is with the patient. The EMT on the engine reports a rapid, thready pulse. The patient, a beautiful 20 something female smiles slightly as I kneel to eye level and gently place two fingers on her wrist to take a radial pulse, which is indeed rapid and thready. “Good afternoon, ma’am.”, I begin, introducing myself. “My name is J, and I’ll be your Medic today. They tell me you’re having palpitations. Has anything like this ever happened before?”, I ask pleasantly. She nods, “Yes, once. I drank too many energy drinks, but I’ve only had a few cups of coffee today.” BINGO. That explains it perfectly. I explain that we need to get going to the hospital and ask if she is okay with being transported. She is, so we assist her to the stretcher and lock it into place in the ambulance. Climbing in, I ask for an assistant from fire with us and with that, the back doors of the ambulance shut.
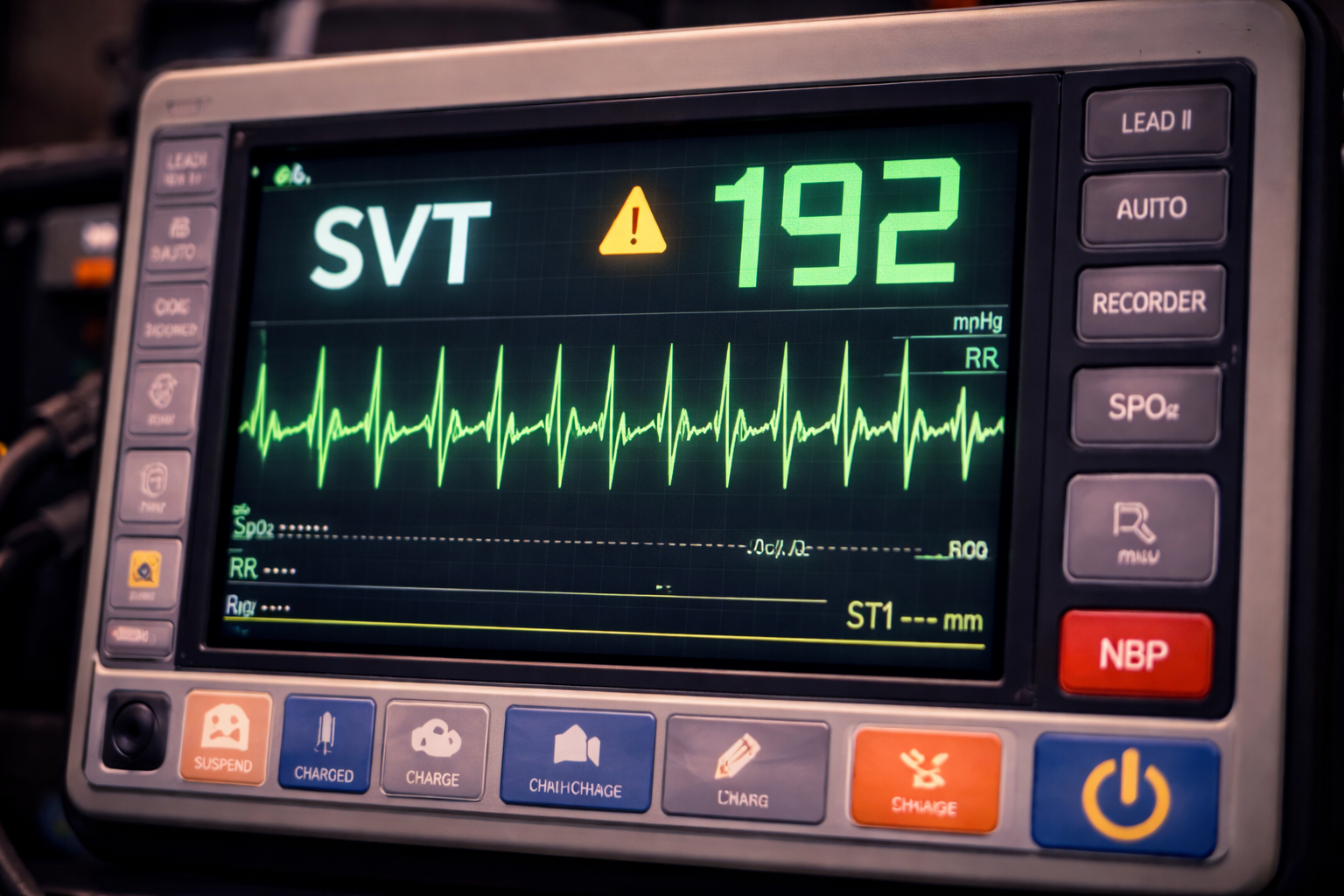
We place our young lady on the cardiac monitor, which shows a rapid, dangerous rhythm called Supraventricular Tachycardia. To explain briefly, it’s a rhythm that is too fast to adequately perfuse (oxygenate) the body, and must be corrected rapidly so as not to deteriorate into cardiac arrest. I smile and tell her about our findings and assure she is in good hands, further explaining as I’m putting defibrillator pads on her chest that some things need to happen first. We share a look, and she asks nervously, “Aren’t those for dead people?”. “No, ma’am”, I assure her, “these are just a fail safe in case the medication I give you doesn’t do the trick. I’m going to give you some Adenosine to slow down that ticker. It’ll make you feel funny, but it should make your heart beat normally.”. She nods and asks that we just get this over with.
I sink a 20 gauge IV into the bend in her left arm and hang a bag of fluids to keep it open. Tabitha has wisely moved to the patient’s right side and is holding her hand to coach her through the hard part. I’ve drawn up the first dose of 6 mg of Adenosine and hand the firefighter a flush to have ready for a rapid flush. “Here we go.”, I say as I push the plunger on the syringe rapidly, the medication entering the patient’s body as the firefighter pushes the flush. A few seconds later, we are awaiting the result…and nothing happens. I draw up another 12 mg of the same medication and tell the patient we’re going to have to do it again. She nods, and the same rapid push and rapid flush happens. This time, her head slumps forward momentarily as her heart rate slows, slows, and slows again to asystole (flat line). What seems like an eternity goes by and just as suddenly as it slowed, it returns to the most beautiful sinus rhythm I’ve ever seen. My patient smiles, deeply sighs, and states she feels much better. Smiling, I nod in agreement as the firefighter and Tabitha step out and close the door, “Alright, that’s what I like to hear. Let’s get you to the hospital.”
As we ride together, we make small talk and I learn that she’s working two jobs to support her two children. She lacks sleep and drinks coffee (much like I do) to keep her sharp and functioning. Transport is uneventful and her rhythm holds, and before I know it, the ambulance slows to a stop. “A couple of bumps getting out.”, I say as we unload the stretcher to take into the hospital. We move her over to the hospital stretcher and I give the doctor a report and hand him the rhythm strip. He pats me on the back and says, “Good job”, and we’re on our way, riding the high of ACTUALLY using my skills to make a difference. Our complete successes are rare, but this one feels like a win. I hop into the passenger seat and we pull from under the awning. Angry static breaks the elation of success as the radio comes to life, “Comms 15, priority one. 9 year old male, cardiac arrest.”. Tabitha and I glance at one another, knowing that the only available ambulance is an intermediate truck and we’re going to get this call anyway. “16 Comms, we’re clear of the hospital, we’ll be en route to that call.”.
This will be my first pediatric cardiac arrest, as I’ve only been a Paramedic for about 3 months. I lean my head back and do the only thing I know to do in this situation…I pray.
To Be Continued with, “Highs and Lows: The Low”.